
In March of 2020, the Webiomed team received an order to add to the system some assessment capabilities for a patient’s coronavirus risk group. We have been closely following the scientific publications on this issue and now we want to share some of the findings with the reader.
A new coronavirus infection became known at the end of 2019. Studying various issues related to COVID-19 requires huge efforts and today in many countries, scientific groups of researchers and entire scientific institutions are working on this problem.
At the moment, about 2,300 clinical studies have been registered, the purpose of which is to obtain reliable scientific information to combat COVID-19.
The results of the studies have clearly shown that COVID-19 is more common and more severe in patients with cardiovascular diseases (CVD).
Discussions are ongoing on many issues related to the contribution of CVD to the burden of COVID-19 severity: the role of risk factors, complications, management tactics and the positive / negative impact of a number of drugs on the development of the disease. Such assessments require large sets of qualitative data.

Previous studies, originally presented by research groups in China, included analysis of 100-200 patients, and of course there were no large randomized trials. However, population studies are necessary to make important clinical and management decisions.
Our team has been working on the issue of coronavirus infection since March 2020. Webiomed CDSS concept implies prediction and stratification by risk groups with prognostic modeling.
All these months, we have been closely monitoring the emerging information about COVID-19. And only in June, six months after the beginning of this epidemic, a paper was published containing an analysis of thousands of patients with CVD and COVID-19. From the sources that we have analyzed, this is the most extensive scientific work, the results of which we would like to share.
The research team analyzed a database of 169 hospitals from Asia, Europe and North America. In included in the study hospitalized COVID-19 patients patients, the association between CVD, drug therapy and in-hospital mortality was assessed. All patients were hospitalized from December 2019 to March 2020.

The observational register included 8,910 patients. Of these, 515 people (5.8%) died in hospital and 8,395 were discharged.
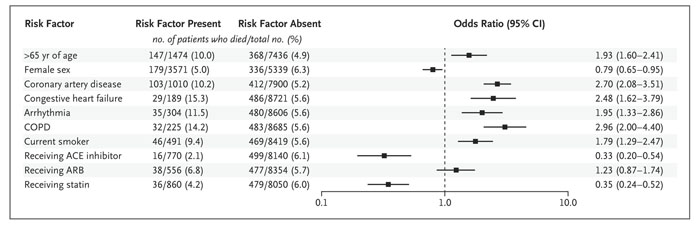
Factors independently associated with an increased risk of in-hospital mortality were:
- age over 65 years (mortality 10.0% vs. 4.9% among patients ≤65 years; odds ratio, 1.93; 95% confidence interval [CI], 1.60-2.41)
- coronary artery disease (10.2% vs. 5.2% among patients without coronary artery disease; odds ratio, 2.70; 95% CI, 2.08-3.51)
- heart failure (15.3% vs. 5.6% among patients without heart failure; odds ratio, 2.48; 95% CI, 1.62-3.79)
- arrhythmia (11.5% vs. 5.6% among patients without arrhythmia; odds ratio, 1.95; 95% CI, 1.33-2.86)
- chronic obstructive pulmonary disease (14.2% vs. 5.6% among patients without COPD; odds ratio, 2.96; 95% CI, 2.00-4.40)
- current smoking (9.4% vs. 5.6% among former smokers or non-smokers; odds ratio, 1.79; 95% CI, 1.29-2.47).
According to the analysis, there was no increase in the risk of in-hospital death with the use of ACE inhibitors (2.1% vs. 6.1%; odds ratio, 0.33; 95% CI, 0.20-0.54) or the use of ARBs (6.8% vs. 5.7%; odds ratio, 1.23; 95% CI, 0.87-1.74).
The results of this study confirm the link between CVD and increased in-hospital mortality among patients with COVID-19, which puts patients with CVD at particular risk.
The study dispels the myth of the association between ACE inhibitors therapy and ARBs therapy and an increased risk of in-hospital mortality once again. Moreover, patients taking ACE inhibitors and statins had better survival rates.
However, the researchers note that these data do not yet provide information on the potential effect of starting an ACE inhibitor or statin therapy in patients with COVID-19 who do not have an appropriate indication for these drugs. Randomized clinical trials will be required to evaluate the role of ACE inhibitors and statins before any conclusion can be reached regarding the potential benefit of these agents in COVID-19 patients.
